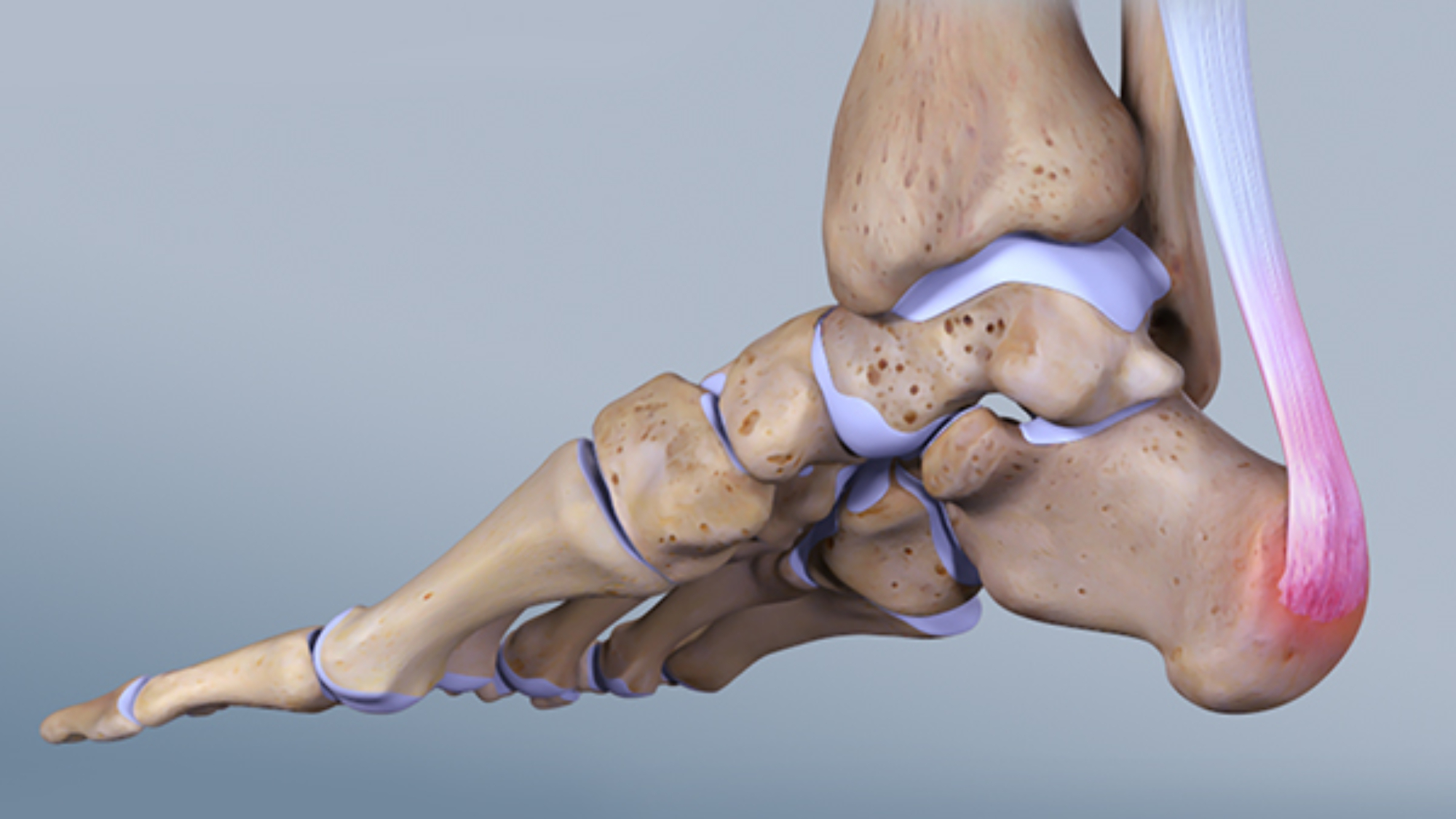
The Achilles tendon, also known as the heel cord, is the tendon that develops at the back of the lower leg that attaches the calf muscles to the heel bone. It is the thickest and strongest tendon in your body and helps cause plantar flexion of your foot at the ankle (raising your heel off the ground).
Achilles tendonitis/tendinitis is a common condition, which occurs when Achilles tendon becomes irritated and inflamed. This condition is associated with overuse and degeneration.
Types of Achilles Tendonitis
There are 2 types of Achilles tendonitis based on the affected part:
· Insertional – This type of Achilles tendonitis affects the lower portion of your heel, where the tendon attaches to the bone of the heel. This type often results in bone spur (extra bone growth) formation.
· Non- Insertional – Non- Insertional tendonitis affects the center portion of the tendon. The fibers herein form tiny tears (degeneration), swell and thicken leading to a sore Achilles tendon or Achilles tendon pain.
Causes of Achilles Tendonitis
Typically, this is not related to any specific injury. It is often the result of repetitive stress to the tendon when you push your body too much, too soon. Your body is unable to repair the injured tissue due to the continual stress. It is for this reason that athletes are highly susceptible to
Achilles tendon disorders.
Other factors also increase oneâs risk of developing this condition. They include a sudden increase in the intensity of physical exercise without proper adaptation, tight calf muscles, tight Achilles tendon, poor biomechanics, excess uphill running and excessive pronation (flattening of the foot arch). Achilles tendonitis is also a side effect of some fluoroquinolone antibiotics such as ciprofloxacin.
Symptoms of Achilles Tendonitis
The most prevalent symptoms of the Achilles tendonitis include:
· Pain, stiffness, swelling, tenderness, and soreness at the Achilles tendon. It can occur at any location along the path of the tendon, starting from the insertion point above your heel to the area below your calf muscles.
· Pain along the tendon that worsens with increased physical activity. The tendon and joint area may become stiffer the next day as the swelling impinges on the tendon movement.
· Thickening of the Achilles tendon when the condition progresses to degeneration.
· Bone spur formation (Insertional tendonitis).
· Intense pain or tenderness when you squeeze the sides of the tendon.
Diagnosis
Achilles tendonitis is usually diagnosed from a physical examination of the tendon and medical history. The podiatrist may order imaging tests to confirm that the symptoms are the result of Achilles tendonitis.
X-ray tests can indicate if there is calcification in the lower portion of the Achilles tendon (an indication of Insertional Achilles tendonitis). The Non-Insertional type can also exhibit calcification in severe cases. Magnetic Resonance Imaging (MRI) while rarely necessary can be ordered in case surgery is planned.
Treatment Options
Non-surgical
Non-surgical treatment of Achilles tendonitis provides pain relief, but it can take some time for the symptoms to subside completely. The options include:
· Rest – The first step in pain alleviation is reducing or ceasing the activities that worsen the pain. Switching from high-impact to low-impact physical activities can reduce the stress on the tendon.
· Ice – Placing ice for up to 20 minutes on the most painful areas of the tendon can reduce the swelling significantly.
· Non-steroidal Anti-inflammatory Medication – NSAIDs such as naproxen and ibuprofen help reduce the pain and swelling.
· Supportive Shoes and Orthotics – Orthotic devices and supportive shoes offer relief from pain caused by insertional Achilles tendonitis. Heel lifts can also take some strain off the Achilles tendon. Frederick Foot and Ankle offers custom orthotic devices and quality special shoes for this purpose.
· Physical Therapy – Physical therapy that includes soft tissue massage/mobilization, eccentric strengthening exercises, ultrasound therapy, gait training/re-education, and stretching is beneficial especially for non-insertional tendonitis.
· Exercise – Some exercises can help in strengthening the calf muscles and reducing the stress placed on the Achilles tendon. They include calf stretches, calf raises, and heel drops.
· Night Splints – Night splints serve to maintain a stretch in the tendon as you sleep.
Surgical Options
Surgery is considered for Achilles tendonitis if the symptoms do not improve after 6 months of non-surgical treatment. At Frederick Foot and Ankle, the podiatrist will select the appropriate surgical procedure based on several factors. They include the location of the tendonitis, amount of tendon damage as well as patient age and activity level.
Achilles Tendonitis prevention is very important. It involves stretching, strengthening exercises and wearing proper shoes for your foot type. If you exhibit any of the symptoms of heel tendonitis, feel free to CONTACT Frederick Foot and Ankle TODAY as early diagnosis and treatment prevents the progression of the condition.

Add a Comment